Current Issue
Climate Change and Skin Health Policy Interventions for Expanding UV Index Alerts, Air Pollution-Induced Dermatoses Awareness, and Subsidized Sunscreen Access in High-Risk Urban Areas
Zahraa Rabeeah1, Alice Kesler2, Therese Limbana3, Shivani S. Ambardekar4, Sanaa Tasneem5, Ramneek Dhami6, Kelly Frasier7*
1Department of Internal Medicine, Piedmont Healthcare, GA, USA
2Department of Medicine, Lakeland Regional Health, Lakeland, FL, USA
3Department of Medical Education, Garnet Health Medical Center, Middletown, USA
4Department of Medicine, University of Illinois at Chicago, Chicago, IL, USA
5Department of Medicine, Marshall University, Huntington, WV, USA
6University of Nevada, Reno School of Medicine, Reno, NV, USA
7Department of Dermatology, Northwell Health, New Hyde Park, NY, USA
*Corresponding author: Kelly Frasier, Department of Dermatology, Northwell Health, New Hyde Park, NY, USA, Phone: 3105956882, E-mail: [email protected]
Received Date: September 05, 2025
Publication Date: April 11, 2026
Citation: Rabeeah Z, et al. (2026). Climate Change and Skin Health Policy Interventions for Expanding UV Index Alerts, Air Pollution-Induced Dermatoses Awareness, and Subsidized Sunscreen Access in High-Risk Urban Areas. Dermis. 6(1):62.
Copyright: Rabeeah Z, et al. © (2026).
ABSTRACT
The growing impact of climate change on skin health necessitates urgent policy interventions aimed at mitigating the risks associated with increased ultraviolet (UV) radiation, air pollution, and limited access to sun protection in high-risk urban populations. Rising global temperatures and the thinning of the ozone layer have led to higher UV radiation exposure, which significantly increases the risk of skin cancer, photoaging, and other UV-induced skin conditions, particularly in urban areas where environmental factors such as pollution exacerbate these risks. Expanding UV index alerts, particularly in high-risk urban environments, is imperative for raising awareness and providing real-time, actionable information to the public, empowering individuals to take preventive measures against harmful UV exposure. In parallel, policy initiatives must address air pollution-induced dermatoses, including conditions such as acne, eczema, and psoriasis, which are aggravated by increased levels of particulate matter, nitrogen dioxide, and other airborne pollutants. Targeted awareness campaigns can educate populations about the detrimental effects of air pollution on skin health, advocating for more stringent air quality regulations and personal protective strategies. Furthermore, subsidized access to sunscreen is an essential policy intervention, as economic barriers often prevent individuals from accessing appropriate sun protection. Implementing programs that provide free or reduced-cost broad-spectrum sunscreens, particularly in high-risk urban areas with disadvantaged populations, would significantly reduce skin cancer risk and improve public health outcomes. By integrating UV index alerts, air pollution awareness, and sunscreen access into cohesive policy frameworks, governments can effectively address the growing challenges posed by climate change on skin health, ensuring that vulnerable populations are better equipped to protect themselves from environmental stressors and reduce long-term skin health burdens.
Keywords: Ultraviolet, Skin Cancer, Greenhouse Gases, Reactive Oxygen Species, Ultraviolet Radiation Index
INTRODUCTION
The World Health Organization warns that climate change threatens to exacerbate health inequities and reverse the past fifty years of progress in development, poverty reduction, and global health [1]. This climate crisis is a direct consequence of human activities that have increased greenhouse gases (GHGs) such as carbon dioxide, methane, and nitrous oxide to unprecedented levels [2]. The resulting elevated temperatures and sea levels have led to natural disasters including frequent and intense heat waves, tropical cyclones, wildfires, and droughts, causing widespread displacement and ecological destruction. In addition to these immediate physical dangers, climate change endangers human health by deteriorating air quality, exacerbating food and water scarcity, increasing the risk of noncommunicable and infectious diseases, and raising psychological stress [1]. These disruptions impact both social determinants of health and health outcomes themselves, with wide-ranging consequences across nearly every organ system.
As the largest organ and primary barrier to the external environment, the skin is uniquely vulnerable to the impacts of climate change. In addition to GHGs warming the climate, the partially depleted ozone layer permits greater skin exposure to ultraviolet radiation, contributing to increased melanoma and nonmelanoma skin cancer risk, among other UV-induced skin conditions [3]. In the United States, nonmelanoma skin cancer incidence has risen sharply since the 1980s, and the incidence of malignant melanoma has tripled over the past four decades. This surge in skin cancers underscores the need for stronger public health interventions as climate changes continue to progress. In addition to skin cancers, air pollutants such as GHGs damage the skin epithelium and exacerbate autoimmune and inflammatory dermatoses, including atopic dermatitis, psoriasis, and acne vulgaris [4]. These risks are not evenly distributed: individuals in lower socioeconomic groups and communities of color often face greater exposure to environmental stressors and encounter barriers to early detection and treatment.
As such, climate change presents a significant public health challenge for skin health, especially among vulnerable populations. Education, public awareness campaigns, and policy reform are urgently needed to mitigate these risks. This manuscript aims to highlight the effects of climate change on skin health and propose policy initiatives to address ultraviolet radiation exposure, air pollution, and inequitable access to sun protection.
REVIEW
Climate Change and Skin Health: The Growing Risk
Ultraviolet (UV) Radiation and Skin Health
The combination of ozone layer depletion and rising global temperatures has led to increased ultraviolet (UV) radiation exposure, significantly impacting skin health. This heightened exposure elevates the risk of skin cancers by causing direct DNA damage and generating reactive oxygen species (ROS) that can lead to mutations and carcinogenesis [4]. Furthermore, chronic UV exposure accelerates the breakdown of collagen and elastin fibers, which contributes to premature photoaging, wrinkles, and hyperpigmentation [5]. Consequently, increasing levels of UV radiation present a dual threat to the skin, simultaneously heightening the danger of malignancy and accelerating the visible signs of aging.
Urban environments pose additional challenges due to the heat island effect, which can intensify UV exposure and its harmful effects on the skin. The combination of increased UV radiation, higher temperatures, and limited access to shade can lead to more severe sunburns and other heat-related skin conditions. As noted by Belzer & Parker [4] and Isler et al. [5], public health initiatives promoting sun protection measures—such as using sunscreen, wearing protective clothing, and seeking shade—are essential to counteract these amplified risks. Therefore, residents of urban areas face a compounded threat from UV radiation that necessitates vigilant and proactive personal protection strategies.
Air Pollution and Dermatoses
Air pollution, which includes particulate matter, nitrogen dioxide, and other contaminants, is increasingly linked to a variety of skin conditions such as acne, eczema, and psoriasis. These pollutants can disrupt the skin barrier, induce oxidative stress, and trigger inflammatory responses that worsen existing dermatoses. According to studies by Çelebi Sözener et al. [6] and Abolhasani et al. [7], pollutants like particulate matter can penetrate the skin to generate ROS, while gaseous pollutants can alter the expression of genes related to skin barrier function. These mechanisms demonstrate how airborne pollutants directly compromise the skin's integrity and inflammatory balance, thereby provoking or exacerbating skin disorders.
The synergistic effects of pollution and climate change further compound these skin health issues, as increased temperatures can enhance the penetration and impact of pollutants while also independently worsening conditions like acne and eczema. This interaction creates a more hostile environment for the skin, contributing to both dermatological diseases and premature aging [8,9]. Addressing these amplified challenges requires a multifaceted approach that combines broad public health efforts to reduce pollution with targeted therapeutic strategies designed to protect and repair the skin barrier.
Policy Interventions and Strategies
UV Index Implementation and Challenges
The ultraviolet radiation index (UVI) was introduced globally to raise awareness and encourage skin protection against skin cancer. A comprehensive review by Heckman et al. of over 20 years of research on the awareness, understanding, use, and impact of the UVI, including 31 studies from the USA, Canada, Europe, Australia, New Zealand, and other regions, reveals mixed results [10]. Awareness of the UVI varies by country, with some showing high awareness. However, understanding and using the UVI to guide sun safety behaviors are generally much lower. In some cases, higher UVI awareness has even been linked to riskier behaviors, such as intentional tanning. It is generally believed that the higher the UVI, the greater the risk for the public to develop diseases linked to excessive UV radiation exposure, although other factors, such as the frequency of exposure to high UV levels, also play a significant role [11].
While the UVI was designed to increase public awareness of the dangers of excessive UV exposure and improve sun protection, global research results have been mixed. Studies from the USA, Canada, Australia, and New Zealand show high levels of awareness, while Europe and other regions have reported lower levels. Some European researchers suggest that the lower UVI in those regions might explain this difference. Regardless of awareness, comprehension of the UVI was consistently lower across all regions [10]. Given the potential negative impact, better education on the UVI and its role in sun protection is needed. Further research is also required to determine how best to communicate UVI information, improve understanding, and enhance its effect on sun protection behaviors. These findings underscore the critical gap between public awareness campaigns and actual behavioral change, suggesting that future UV index initiatives must move beyond simple information dissemination to include comprehensive education about risk assessment and practical implementation strategies.
Air Pollution Awareness and Communication
Accurate and timely information can be a powerful tool in reducing the harmful effects of air pollution. Although national guidelines for environmental risk communication, based on risk and crisis communication principles, are available, little is known about how these guidelines are implemented or the effectiveness of current communication efforts. Additionally, the expanding literature on environmental health literacy indicates that communication about environmental risks should go beyond educating individuals on behavior and focus on empowering communities to take action to reduce environmental threats [12].
The widespread impact of air pollution highlights the importance of environmental justice, as marginalized communities bear a disproportionate share of poor air quality. Implementing clean air policies benefits public health and promotes social equity by ensuring all populations have access to safer, cleaner air. Additionally, the economic burden of healthcare costs related to treating the long-term effects of air pollution emphasizes the need for immediate action to prevent these diseases at their source. Global efforts to reduce emissions from industries and invest in cleaner, renewable energy sources are vital steps in mitigating the impact of air pollution and protecting future generations [13]. These systemic approaches must be coupled with immediate protective interventions to bridge the gap between long-term policy change and current health needs, particularly for communities already experiencing the highest exposure burdens.
Sunscreen Access and Regulation
Sunscreens are topical products with ultraviolet filters (UVFs). While sunscreen regulation has increased in the U.S., we still have fewer UVF options compared to other countries. Effective sun protection to prevent skin cancer and aging includes sun avoidance, protective clothing, and sunscreen use [14]. IMPACT Melanoma analyzed and compared melanoma distribution data from 2020-2021 with records from 2018-2019. Healthcare facilities, public health departments, governmental organizations, parks, educational institutions, nonprofits, and private businesses all ordered sunscreen dispensers and various sunscreen types for public use. Across all sectors, there was a significant decline in orders, with sunscreen dispenser orders decreasing by 58% and sunscreen cases by 68%. Park and recreation centers, along with nonprofits—who were the top orders in 2018-2019—saw decreases of 78% and 42%, respectively, from 2020-2021. Despite widespread supply chain disruptions, sunscreen availability remained intact, with hybrid sunscreens being the most frequently ordered. Chemical and physical sunscreens were not ordered in 2020-2021, possibly due to their declining popularity. IMPACT Melanoma's touch-free automated sunscreen dispensers and robust virtual outreach programs will be key in addressing this decline [15]. These dramatic reductions in sunscreen distribution highlight the vulnerability of existing public health infrastructure during crisis periods and underscore the need for more resilient, crisis-resistant distribution systems that can maintain protective resource availability regardless of external circumstances.
Integrated Policy Framework for Skin Health
The detrimental effects of ultraviolet (UV) radiation are significantly amplified by air pollution, acting synergistically to exacerbate oxidative stress, DNA damage, and inflammation. This potent combination accelerates skin aging and increases the risk of carcinogenesis, not only through direct cellular damage but also by promoting immune dysregulation and the accelerated breakdown of collagen and elastin [16]. Demonstrating the joint adverse effects of UV and pollution, Soeur et al. identified that UVA1 induction of trace amounts of polyaromatic hydrocarbons significantly impairs keratinocyte viability by producing high levels of cellular stress [17]. Further supporting this synergistic relationship, Vierköter et al.'s research demonstrated clinically that even minor increases in traffic-related particulate matter, a key component of air pollution, correlated with a greater prevalence of UV-induced lentigines and deeper wrinkles in women [18]. Similarly, Flament et al.'s findings in Chinese women exposed to polluted air mirrored these outcomes, showing exacerbated changes in skin texture and color indicative of accelerated aging driven by this combined environmental assault [19]. Therefore, ensuring broad and equitable access to sunscreen is a vital public health measure to help individuals protect themselves against this amplified environmental threat to skin health.
Adopting a cohesive and comprehensive approach integrating expanded UV index alerts, air pollution awareness campaigns, and subsidized sunscreen access offers significant benefits. By simultaneously addressing the combined harm of UV radiation and air pollution, these policies can more effectively reduce skin cancer incidence and pollution-related skin conditions. Educating the public about both risks and improving access to protective measures empowers individuals to make informed preventative choices regarding outdoor activities and sunscreen use. Furthermore, integrating these initiatives streamlines resource allocation by leveraging shared distribution networks and outreach programs. This integrated framework ensures broader dissemination of vital information across communities, regardless of socioeconomic status, equipping them with the knowledge and tools for skin protection and fostering the adoption of sun-safe and pollution-conscious behaviors.
Implementing these strategies presents several significant hurdles that demand careful consideration and proactive solutions. A primary challenge involves coordination and collaboration across diverse sectors. Ineffective alignment among governmental agencies, non-profit organizations, and community stakeholders can fragment funding, create inconsistent public messaging, and result in unequal access to crucial information and resources. Navigating these partnerships and ensuring clear communication are fundamental for successful policy implementation. Furthermore, public skepticism and misinformation present additional substantial obstacles [20]. This skepticism, potentially stemming from a general distrust of scientific findings or government recommendations, can lead individuals to underestimate the combined risks of UV radiation and air pollution [21]. Exacerbating this issue are misinformation campaigns, potentially amplified by lobbying efforts from industries facing stricter air quality regulations. These campaigns can erode public trust [22] and create resistance to adopting recommended protective behaviors, ultimately undermining the intended impact of the integrated skin health policy. Addressing this requires proactive and culturally sensitive communication strategies that build trust, clearly articulate the scientific evidence, and counter misinformation with accurate and accessible information.
Addressing Skin Health in the Era of Climate Change
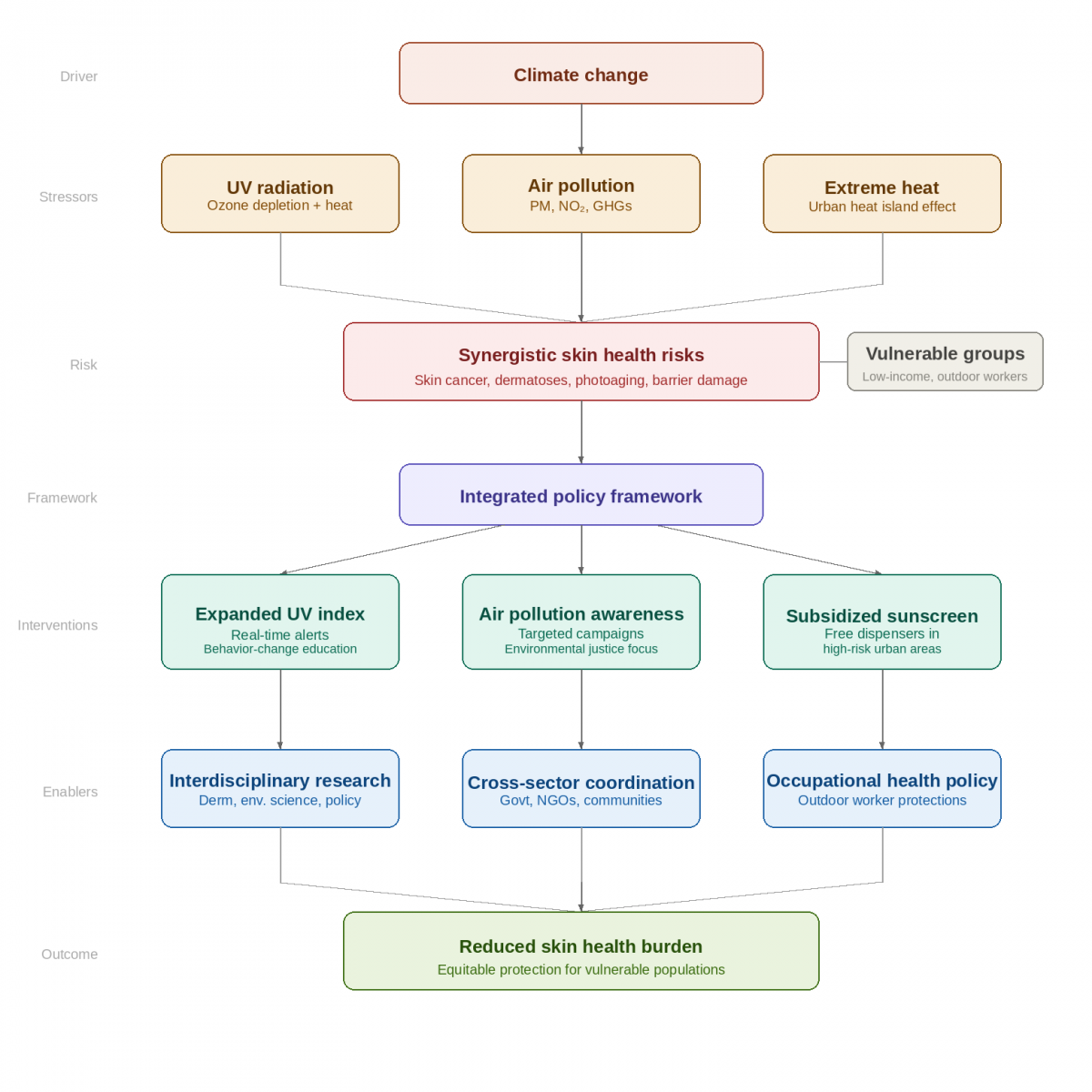
Climate change is becoming increasingly recognized as one of the main drivers of dermatologic disease. Exposures such as UV radiation, air pollution, and extreme weather worsen conditions such as atopic dermatitis [23]. Rising temperatures and fluctuating humidity levels leave skin barriers compromised, which makes individuals more susceptible to irritants and allergens [24]. Poor skin health also has broader consequences such as increased work absenteeism, decreased productivity, and increased healthcare costs [25]. However, vulnerable populations bear a disproportionate burden of climate-related skin health risks such as outdoor workers and low-income groups [23]. Higher-risk populations may face additional pressures due to harsher environmental exposures, leading to a strain on the public health systems due to the increasing prevalence of skin disease, especially when it comes to underserved areas. Without proactive and proper intervention, health inequities will continue to grow. Additionally, interdisciplinary collaboration between dermatology, environmental science, occupational health, and public policy in integrated care models is essential for developing effective solutions [23,26]. This collaborative approach represents a fundamental shift from traditional siloed medical practice toward comprehensive care models that recognize the complex interplay between environmental factors and health outcomes (Figure 1).
Figure 1: Flow Chart Showing Effect of Climate Change on Skin Health
Future Research
Despite the rising acknowledgment of climate change on skin health, major gaps in research remain. For example, there is an urgent need for more longitudinal research on the cumulative impact of environmental exposures [23,24]. This is especially true in areas such as how pollutants and the earth's ozone interact to break down the skin's barrier [23]. Further research is also needed to fully realize how climate-driven changes alter the skin's microbiome in influencing disease susceptibility and how innovative strategies and integrated care pathways can be used to mitigate these risks [23,25,26]. Additionally, teledermatology presents a promising but underexplored method for delivering skin-related healthcare to vulnerable populations and those most affected by climate-related risks [26]. Lastly, pediatric and geriatric populations—who are particularly sensitive to environmental stressors—deserve dedicated longitudinal research to ensure equitable skin health outcomes under future climate conditions [23,24]. These critical knowledge gaps must be addressed to inform policy recommendations and develop evidence-based interventions capable of protecting the most vulnerable populations while advancing our understanding of climate-health interactions in dermatological care.
CONCLUSION
The intersection of climate change and dermatological health represents a significant public health challenge that requires comprehensive policy intervention. The evidence demonstrates that rising UV radiation exposure and air pollution are creating synergistic threats to skin health that disproportionately impact vulnerable populations, including outdoor workers, low-income communities, and communities of color. Current approaches to UV protection, air quality management, and sunscreen access, while valuable, remain fragmented and insufficient to address the complex, interconnected nature of these environmental health challenges. An integrated policy framework that simultaneously addresses multiple environmental stressors while ensuring equitable access to protective resources offers the most promising path forward. By implementing expanded UV index alert systems, comprehensive air pollution awareness campaigns, and subsidized sunscreen access programs within a unified approach, policymakers can create meaningful protection for those most at risk while building more resilient public health infrastructure. The research presented in this manuscript highlights both the urgency of these challenges and the availability of evidence-based solutions that can effectively mitigate climate-related skin health risks while promoting health equity across diverse populations.
REFERENCES
- WHO. (2023). Climate change. World Health Association.
- Climate change 2021: The physical science basis: summary for policymakers: working group I contribution to the sixth Assessment report of the Intergovernmental Panel on Climate Change (with Masson-Delmotte, V., Zhai, P., & Pirani, A.). (2021). IPCC.
- Parker ER. (2021). The influence of climate change on skin cancer incidence – A review of the evidence. International Journal of Women’s Dermatology, 7(1):17-27.
- Belzer A, Parker ER. (2023). Climate Change, Skin Health, and Dermatologic Disease: A Guide for the Dermatologist. American Journal of Clinical Dermatology. 24(4):577-593.
- Isler MF, Coates SJ, Boos MD. (2023). Climate change, the cutaneous microbiome and skin disease: Implications for a warming world. International Journal of Dermatology. 62(3):337-345.
- Çelebi Sözener Z, Treffeisen ER, Özdel Öztürk B, Schneider LC. (2023). Global warming and implications for epithelial barrier disruption and respiratory and dermatologic allergic diseases. The Journal of Allergy and Clinical Immunology. 152(5):1033-1046.
- Abolhasani R, Araghi F, Tabary M, Aryannejad A, Mashinchi B, Robati RM. et al. (2021). The impact of air pollution on skin and related disorders: A comprehensive review. Dermatologic Therapy. 34(2):e14840.
- Passeron T, Krutmann J, Andersen ML, Katta R, Zouboulis CC. (2020). Clinical and biological impact of the exposome on the skin. Journal of the European Academy of Dermatology and Venereology. 34(Suppl 4):4-25.
- Ali A, Khan H, Bahadar R, Riaz A, Asad MHHB. (2020). The impact of airborne pollution and exposure to solar ultraviolet radiation on skin: Mechanistic and physiological insight. Environmental Science and Pollution Research International. 27(23):28730-28736.
- Heckman CJ, Liang, K, Riley M. (2019). Awareness, understanding, use, and impact of the UV index: A systematic review of over two decades of international research. Prev Med. 123:71-83.
- Twilley D, Rademan S, Lall N. (2018). Chapter 2 - Are Medicinal Plants Effective for Skin Cancer? In N. Lall (Ed.), Medicinal Plants for Holistic Health and Well-Being (pp. 13-75). Academic Press.
- Ramírez AS, Ramondt S, Van Bogart K, Perez-Zuniga R. (2019). Public Awareness of Air Pollution and Health Threats: Challenges and Opportunities for Communication Strategies To Improve Environmental Health Literacy. Journal of Health Communication. 24(1):75-83.
- Chen F, Zhang W, Mfarrej MFB, Saleem MH, Khan KA, Ma J, et al. (2024). Breathing in danger: Understanding the multifaceted impact of air pollution on health impacts. Ecotoxicology and Environmental Safety. 280:116532.
- Sabzevari N, Qiblawi S, Norton SA, Fivenson D. (2021). Sunscreens: UV filters to protect us: Part 1: Changing regulations and choices for optimal sun protection. International Journal of Women's Dermatology. 7(1):28-44.
- Szeto MD, Kokoska RE, Maghfour J, Rundle CW, Presley CL, Harp T. (2022). An analysis of public sunscreen distribution in the United States during the COVID-19 pandemic. Journal of the American Academy of Dermatology. 86(5):e241-e243.
- Papaccio F, D Arino A, Caputo S, Bellei B. (2022). Focus on the contribution of oxidative stress in skin aging. Antioxidants, 11(6):1121.
- Soeur J, Belaïdi JP, Chollet C, Denat L, Dimitrov A, Jones C. (2017). Photo-pollution stress in skin: Traces of pollutants (PAH and particulate matter) impair redox homeostasis in keratinocytes exposed to UVA1. Journal of Dermatological Science. 86(2):162-169.
- Vierkötter A, Schikowski T, Ranft U, Sugiri D, Matsui M, Krämer U, et al. (2010). Airborne particle exposure and extrinsic skin aging. Journal of Investigative Dermatology. 130(12):2719–2726.
- Flament F, Bourokba N, Nouveau S, Li J, Charbonneau A. (2018). A severe chronic outdoor urban pollution alters some facial aging signs in Chinese women. A tale of two cities. International Journal of Cosmetic Science. 40(5):467-481.
- Treen KMD, Williams HTP, O’Neill SJ. (2020). Online misinformation about climate change. Wiley Interdisciplinary Reviews Climate Change. 11(5):11:e665.
- Zhou M. (2014). Public environmental skepticism: A cross-national and multilevel analysis. International Sociology. 30(1):61–85.
- Brulle RJ, J.,Roberts JT. (2017). Climate misinformation campaigns and public sociology. Contexts. 16(1):78–79.
- Wang SP, Stefanovic N, Orfali RL, Aoki V, Brown SJ, Dhar S, et al. (2024). Impact of climate change on atopic dermatitis: A review by the International Eczema Council. Allergy, 79(6):1455–1469.
- Engebretsen KA, Johansen JD, Kezic S, Linneberg A, Thyssen JP. (2016). The effect of environmental humidity and temperature on skin barrier function and dermatitis. Journal of the European Academy of Dermatology and Venereology, 30(2):223–249.
- Lampel HP, Powell HB. (2019). Occupational and Hand Dermatitis: A Practical Approach. Clinical Reviews in Allergy & Immunology. 56(1):60–71.
- Zuberbier T, Abdul Latiff A, Aggelidis X, Augustin M, Balan RG, Bangert C, et al. (2023). A concept for integrated care pathways for atopic dermatitis—A GA2LEN ADCARE initiative. Clinical and Translational Allergy. 13(9):e12299.
 Abstract
Abstract  PDF
PDF