Past Issues
Angiosarcoma on Paralytic Lower Limb: A Rare Form of Stewart-Treves Syndrome
Taibi-Berrah Lynda*
Dermatology Clinic, Mustapha University Hospital, Algiers; University of Medicine of Algiers
*Corresponding Author: Taibi-Berrah L, Dermatology Clinic, Mustapha University Hospital, Algiers; University of Medicine of Algiers; Email: [email protected]
Received Date: February 29, 2024
Publication Date: March 20, 2024
Citation: Taibi-Berrah L. (2024). Angiosarcoma on Paralytic Lower Limb: A Rare Form of Stewart-Treves Syndrome. Dermis. 4(1):8.
Copyright : Taibi-Berrah L. © (2024).
ABSTRACT
Stewart-Treves syndrome is a rare disease defined by the occurrence of angiosarcoma in chronic lymphedema. Its management remains difficult combined to a poor prognosis. Causes of this syndrome are dominated by the surgical treatment of cancers but other, rarer causes of lymphedema may be responsible. It is then either of congenital origin or occurs on a post-traumatic paralyzed limb.
INTRODUCTION
Angiosarcoma is a rare, aggressive vascular malignancy with a poor prognosis. Primary cutaneous angiosarcoma arises de novo on the head and neck of the elderly, whereas secondary angiosarcoma, referred to as Stewart-Treves syndrome, arises on upper or lower limbs in the setting of chronic lymphedema or previous irradiation [1].
We report a case of angiosarcoma arising in the right lower limb of a patient suffering from post-traumatic tetraplegia dating back 25 years.
CASE REPORT
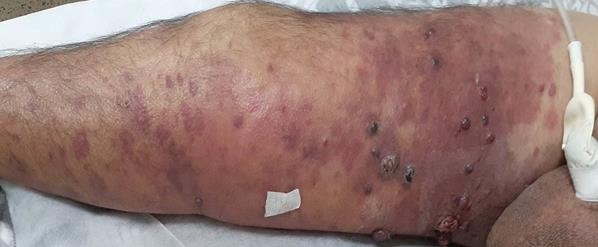
A 53-year-old man, with C6 motor tetraplegia for 25 years following a road accident, was admitted to the dermatology department for angiomatous lesions of the right lower limb that had appeared 8 months ago. Dermatological examination revealed multiple macular lesions, red to purplish that do not disappear with vitropressure, warm, isolated or grouped in infiltrated patches running along the entire thigh and leg up to the ankle, and mixed together multiple firm purplish popular and nodular lesions, 0.5 to 2 cm in diameter, with a keratotic or ulcerated surface, located circumferentially around the right thigh. Lymphedema of the same limb was noted as well as ipsilateral scrotal oedema.
No particular abnormality was found in the biological assessment. Arterial and venous Doppler ultrasound was normal and standard radiography did not reveal any bone lesions or suspicious condensation. A moderate hydrocele was visualized on scrotal ultrasound.
Figure: Angiomatous lesions of the right lower limb.
Skin biopsy specimen revealed beneath a regular epidermis, a fibrous dermis with diffuse and poorly limited vascular proliferation, made of spindle cells on the first biopsy and globular cells with clear nuclei with the presence of some mitotic images and focal extravasated red blood cells. Immunohistochemistry showed negative HHV8 staining, CD34 positivity and intense and diffuse ERG (erythroblast transformation-specific related gene) and CD31 positivity. These aspects led to the diagnosis of angiosarcoma being retained.
The histological and clinical comparison argued in favour of a steward-Treves syndrome in the form of secondary angiosarcoma in the context of lymphedema on a paralytic limb.
The initial extension assessment including a thoraco-abdominopelvic CT scan and an upper digestive endoscopy did not reveal any metastatic locations. The extent of the lesions and the rapid deterioration of the patient’s general condition did not allow amputation to be proposed, and despite a slight melting of the lesions obtained by the initiation of chemotherapy with bleomycin then vinblastine, the death of the patient in a picture of acute respiratory distress quickly occurred in less than two months after the diagnosis was made.
DISCUSSION
Soft tissue sarcomas represent less than 1% of all malignant tumours. Among them, only 2% correspond to angiosarcomas [2]. STS represents between 5% and 8% of sarcomas [3-4].
The first described Stewart-Treves syndrome STS cases in 1948, corresponded to angiosarcomas occurring in lymphedema after mastectomy with curative intent for breast cancer, associated or not with radiotherapy [5]. However, it seems that a previous observation already mentioned angiosarcoma on lymphedema in 1906 on post-traumatic lymphedema [6].
Our patient’s history and the clinical and histological aspects with the description of spindle cells on the first biopsy and globular cells on the second one, the deep dermis invasion, the numerous mitotic figures, extravasated red blood cells and a tumour which demonstrated strong erythroblast transformation specific related gene ERG nuclear positivity, which is highly specific for vascular tumours and highly sensitive for angiosarcoma [7]. All of the collected information supports the diagnosis of angiosarcoma on a post- traumatic paralytic limb.
The rapid spread of the lesions, the difficulty of treatment and the terrible prognosis are mentioned in the rare cases published in the medical literature [8,9].
The mechanism by which lymphedema induces tumorigenesis in STS is not fully understood. It may be caused by impaired lymphatic drainage that disrupts immune cell trafficking and creates an environment inept at recognizing and destroying tumour cells [1].
It is further suggested that lymphatic stasis to be responsible for a strong stimulation of angiogenesis via secreted growth factors for the production of collateral lymphatic and vascular channels 1 seems to be highly associated with secondary angiosarcoma [1,8,10].
In patients suffering from paraplegia or quadriplegia, muscular paralysis combined with their reduced mobility makes them particularly vulnerable to the development of lymphedema [11]. The complications that can then follow are diverse, ranging from infection or skin ulceration to the development of cancer, as shown in our case.
CONCLUSION
Our case, showing Stewart-Treves syndrome (angiosarcoma on lymphoedema) in a post-traumatic paralytic limb, highlights the need for physicians caring for patients with paralysis, to be particularly vigilant during the clinical skin examination, of such unusual aspects or modifications in the integument.
REFERENCES
- Lee R, Saardi KM, Schwartz RA. (2014). Lymphedema-related angiogenic tumors and other malignancies. Clin Dermatol. 32: 616-620.
- Mark RJ, Poen JC, Tran LM, FU YS, Juillard GF. (1996). Angiosarcoma: A report of 67 patients and a review of the literature. Cancer. 77; 2400-2406.
- Buehler D, Rice SR, Moody JS, Rush P, Hafez GR, Attia S, et al. (2014). Angiosarcoma outcomes and prognostic factors: a 25-years institution experience. Am J Clin Oncol. 37:473-479.
- Fayette J, Martin E, Piperno-Neumann S, Le Cesne A, Robert C, Bonvalot S, et al. (2007). Angisarcomas, a heterogenous group of sarcomas with specific behavior depending on primary site: a retrospective study of 161 cases. Ann Oncol Off J Eur Soc Med Oncol. 18: 2030-2036.
- Stewart FW, Treves N. (1948). Lymphangisarcoma in postmastectomy lymphedema. A report of six cases in elephantiasis chirurgica. Cancer. 1:64-81
- Lowenstein S. (1906). Der atiologische zusammenhang zwischen akutem ein-maligem trauma and sarkon. Z Klin Clir. 48:780-824.
- Sullivan HC, Edgar MA, Cohen C. (2015). The utility of ERG, CD31 and CD34 in the cytological diagnosis of angiosarcoma: an analysis of 25 cases. J Clin Pathol. 68:44-50.
- Fischer AS, Rizk C, Sutton L, Krishnan B, Orengo I, Cohen DN. (2017). Stewart-Treves syndrome in a spinal cord injury patient with MYC amplification. JAAD Case Rep. 3(6):515-518.
- Krich S, Mernissi FZ. (2016). Syndrome de Stewart-Treves: complication rare de lymphoedème chronique. Pan Afr Med J. 24:196.
- Turquier E, Chantalat L, Fourgeaud C, Vignes S. (2022). Syndrome de Stewart-Treves. Dermat Vénérol. (2022):183-191.
- Jain NB, Ayers GD, Peterson EN, Harris MB, Morse L, O'Connor KC, et al. (2015). Traumatic spinal cord injury in the United States. 1993-2012. JAMA. 313: 2236-2243.
 Abstract
Abstract  PDF
PDF